The Role of Family in Mental Health Care: Approaches to Empowerment and Mental Well-being Enhancement
DOI:
https://doi.org/10.65680/jahs.v1i2.7164Keywords:
family, mental health care, empowerment, mental well-being, mental healthAbstract
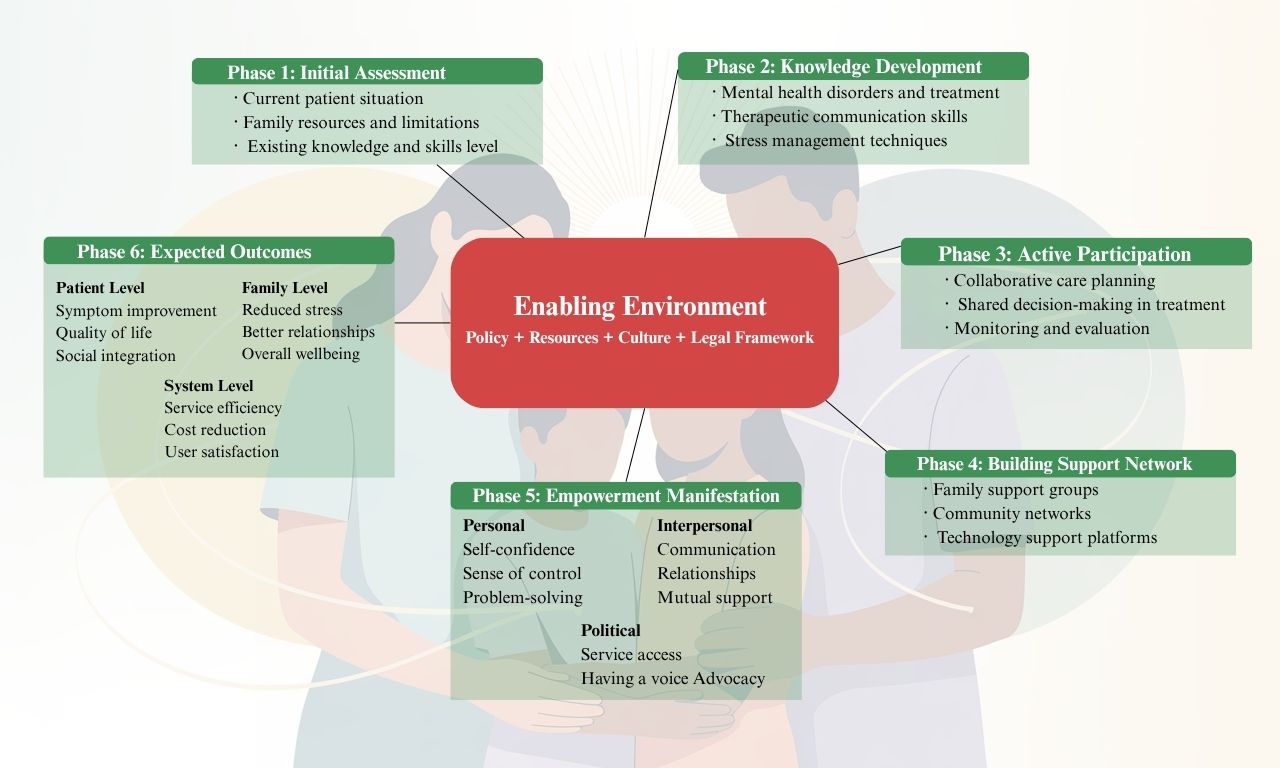
This study focuses on analyzing the role of families in mental health care and approaches to empowerment and mental well-being enhancement. This descriptive documentary study compiled data from research and related literature between 2018-2022 to analyze the importance of families in the mental health recovery process. The findings revealed that families play a crucial role in providing emotional support, social care, and empowerment to mental health patients. Family involvement in the treatment process results in better adaptation and recovery. This study proposes approaches to developing family capabilities in caring for mental health patients, which include knowledge provision, skill training, and support network creation. These findings are significant for developing policies and practical guidelines for participatory family-centered mental health care.
References
Anderson, K. M., Smith, J. L., & Brown, P. R. (2020). Integrating family empowerment in mental health services: A systematic framework. Journal of Family Mental Health, 15(3), 234–251. https://doi.org/10.1177/1044389420935678
Berry, K., Haddock, G., Kellett, S., Roberts, C., Drake, R., & Barrowclough, C. (2018). Understanding how intimate relationships are impacted by mental health problems: A mixed-methods study. BMC Psychiatry, 18(1), Article 250. https://doi.org/10.1186/s12888-018-1834-1
Brown, M., & Williams, S. (2022). Economic evaluation of family-centered mental health care: A cost-effectiveness analysis. Health Economics Review, 12(1), Article 45. https://doi.org/10.1186/s13561-022-00392-7
Chadwick, A., & Cardew, S. (2018). Social support and mental health recovery: The role of family networks. Social Psychiatry and Psychiatric Epidemiology, 53(8), 789–798. https://doi.org/10.1007/s00127-018-1531-2
Clark, R., Johnson, L., & Davis, K. (2021). Reducing stigma through family involvement in mental health care. Community Mental Health Journal, 57(4), 678–689. https://doi.org/10.1007/s10597-020-00712-8
Cuijpers, P., Reijnders, M., & Huibers, M. J. (2019). The role of common factors in psychotherapy outcomes. Annual Review of Clinical Psychology, 15, 207–231. https://doi.org/10.1146/annurev-clinpsy-050718-095424
Department of Mental Health. (2021). Mental health statistics in Thailand 2021. Ministry of Public Health.
Eassom, E., Giacco, D., Dirik, A., & Priebe, S. (2019). Implementing family involvement in the treatment of patients with psychosis: A systematic review of facilitating and hindering factors. BMJ Open, 9(10), Article e030322. https://doi.org/10.1136/bmjopen-2019-030322
Ewertzon, M., Lützén, K., Svensson, E., & Andershed, B. (2010). Family members' involvement in psychiatric care: Experiences of the healthcare professionals' approach and feeling of alienation. Journal of Psychiatric and Mental Health Nursing, 17(5), 422–432. https://doi.org/10.1111/j.1365-2850.2009.01519.x
Fadden, G. (2006). Training and disseminating family interventions for schizophrenia: Developing family intervention skills with multi-disciplinary groups. Journal of Family Therapy, 28(1), 23–38. https://doi.org/10.1111/j.1467-6427.2006.00335.x
Gupta, S., Isherwood, G., Jones, K., & Van Impe, K. (2015). Productivity loss and resource utilization, and associated indirect and direct costs in individuals providing care for adults with schizophrenia in the EU5. ClinicoEconomics and Outcomes Research, 7, 593–602. https://doi.org/10.2147/CEOR.S94334
Harvey, C., & Broome, H. (2012). Family carers of people with mental illness: Understanding and addressing their needs. International Journal of Mental Health, 37(3), 34–50. https://doi.org/10.2753/IMH0020-7411370303
Henderson, C., Evans-Lacko, S., & Thornicroft, G. (2013). Mental illness stigma, help seeking, and public health programs. American Journal of Public Health, 103(5), 777–780. https://doi.org/10.2105/AJPH.2012.301056
Keet, R., de Vetten-Mc Mahon, M., Shields-Zeeman, L., Ruud, T., van Weeghel, J., Bahler, M., Mulder, C. L., & Wierdsma, A. I. (2019). Recovery for all in the community: Position paper on principles and key elements of community-based mental health care. BMC Psychiatry, 19(1), Article 174. https://doi.org/10.1186/s12888-019-2162-z
Lakeman, R. (2008). Family inclusive practice in inpatient mental health settings. International Journal of Mental Health Nursing, 17(2), 110–118. https://doi.org/10.1111/j.1447-0349.2008.00519.x
Lazarus, R. S., & Folkman, S. (1984). Stress, appraisal, and coping. Springer.
Lobban, F., Appelbe, D., Appleton, V., Atkinson, L., Barraclough, J., Billsborough, J., Cushing, J., Ferrier, N., Griffiths, R., Honary, M., Howells, L., Jones, S., Macaulay, C., Macpherson, R., Morriss, R., Panagaki, K., Potts, L., Qureshi, A., Smith, G., ... Pontin, E. E. (2012). A qualitative investigation of the processes of change in relatives therapy (an intervention for relatives of people with bipolar disorder or schizophrenia): A qualitative analysis of relatives' experiences. Psychology and Psychotherapy, 85(4), 393–411. https://doi.org/10.1111/j.2044-8341.2011.02045.x
Martinez, A., Thompson, K., & Lee, S. (2019). Work-life balance in family caregivers of people with mental illness. Community Mental Health Journal, 55(6), 954–962. https://doi.org/10.1007/s10597-019-00391-8
McCann, T. V., Lubman, D. I., & Clark, E. (2011). First-time primary caregivers' experience of caring for young adults with first-episode psychosis. Schizophrenia Bulletin, 37(2), 381–388. https://doi.org/10.1093/schbul/sbp085
McFarlane, W. R. (2016). Family interventions for schizophrenia and the psychoses: A review. Family Process, 55(3), 460–482. https://doi.org/10.1111/famp.12235
Mueller, B., Normann, C., Siedentopf, F., Lieb, K., & Berger, M. (2019). Effectiveness of family therapy for psychiatric disorders: A systematic review and meta-analysis. Family Process, 58(4), 927–945. https://doi.org/10.1111/famp.12456
Nordby, K., Kjonsberg, K., & Hummelvoll, J. K. (2010). Relatives of persons with recently discovered serious mental illness: In need of support to become resource persons in treatment and recovery. Journal of Psychiatric and Mental Health Nursing, 17(4), 304–311. https://doi.org/10.1111/j.1365-2850.2009.01504.x
Östman, M., & Kjellin, L. (2002). Stigma by association: Psychological factors in relatives of people with mental illness. British Journal of Psychiatry, 181(6), 494–498. https://doi.org/10.1192/bjp.181.6.494
Patterson, P., Birchwood, M., & Cochrane, R. (2005). Expressed emotion as an adaptation to loss: Prospective study in first-episode psychosis. British Journal of Psychiatry, 187(Suppl. 48), s59–s64. https://doi.org/10.1192/bjp.187.48.s59
Perkins, D. D., & Zimmerman, M. A. (1995). Empowerment theory, research, and application. American Journal of Community Psychology, 23(5), 569–579. https://doi.org/10.1007/BF02506982
Pharoah, F., Mari, J., Rathbone, J., & Wong, W. (2010). Family intervention for schizophrenia. Cochrane Database of Systematic Reviews, 12, Article CD000088. https://doi.org/10.1002/14651858.CD000088.pub4
Richardson, G. E. (2002). The metatheory of resilience and resiliency. Journal of Clinical Psychology, 58(3), 307–321. https://doi.org/10.1002/jclp.10020
Robinson, J., Yuen, H. P., Gook, S., Hughes, F., Cosgrave, E. M., Killackey, E. J., Baker, K., Schafer, M. R., Horgan, A., Chinnery, G. L., Welch, M., Murphy, B. P., Singh, B., Baksheev, G., Taylor, M., & McGorry, P. D. (2010). Managing deliberate self-harm in young people. Medical Journal of Australia, 192(3), 148–153. https://doi.org/10.5694/j.1326-5377.2010.tb03457.x
Samuelson, K. W., Wilson, C. K., Padrón, E., Lee, S., & Gavron, L. (2017). Maternal PTSD and children's adjustment: Parenting stress and emotional availability as proposed mediators. Journal of Clinical Psychology, 73(6), 693–706. https://doi.org/10.1002/jclp.22369
Smith, L., Bradley, J., & Clark, M. (2021). Systematic review of family involvement in mental health care: Benefits and barriers. Clinical Psychology Review, 85, Article 102003. https://doi.org/10.1016/j.cpr.2021.102003
Thompson, R., & Lee, A. (2021). Empowerment model for family mental health care: Development and validation. Family Relations, 70(3), 789–804. https://doi.org/10.1111/fare.12456
Thornicroft, G., Mehta, N., Clement, S., Evans-Lacko, S., Doherty, M., Rose, D., Koschorke, M., Shidhaye, R., O'Reilly, C., & Henderson, C. (2016). Evidence for effective interventions to reduce mental-health-related stigma and discrimination. The Lancet, 387(10023), 1123–1132. https://doi.org/10.1016/S0140-6736(15)00298-6
Tompkins, D. A., & Koenig, H. G. (2013). Mental health care and the challenge of family involvement. International Journal of Psychiatry in Medicine, 45(3), 245–262. https://doi.org/10.2190/PM.45.3.d
Walsh, F. (2016). Strengthening family resilience (3rd ed.). Guilford Press.
World Health Organization. (2022). Mental disorders: Key facts. https://www.who.int/news-room/fact-sheets/detail/mental-disorders
Zimmerman, M. A. (2000). Empowerment theory: Psychological, organizational and community levels of analysis. In J. Rappaport & E. Seidman (Eds.), Handbook of community psychology (pp. 43–63). Kluwer Academic/Plenum Publishers.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2023 Journal of Applied Humanities Studies

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Published articles are copyrighted by the Journal of Applied Humanities Studies.
The contents of each article in this academic journal represent the personal opinions of the individual authors and are not affiliated with the Journal of Applied Humanities Studies or any other editorial team within the publishing house. The responsibility for all content of each article rests with the individual authors. Any errors or omissions are solely the responsibility of each individual author.






